INTRODUCING
ClaimPilot
Generative AI for Payment Integrity
INTRODUCING
ClaimPilot
Generative AI for Payment Integrity
Looking for a copilot for your payment integrity team?
Codoxo is at the forefront of a movement that will not only help healthcare payers and agencies but will also impact the greater good of the healthcare system. Every year, billions of dollars are lost to fraud, waste and abuse. We see a better way. You need a partner who is acting today to solve tomorrow’s most pressing issues. We invite you to join us in making an impact on healthcare affordability and effectiveness. That’s seeing tomorrow, today.
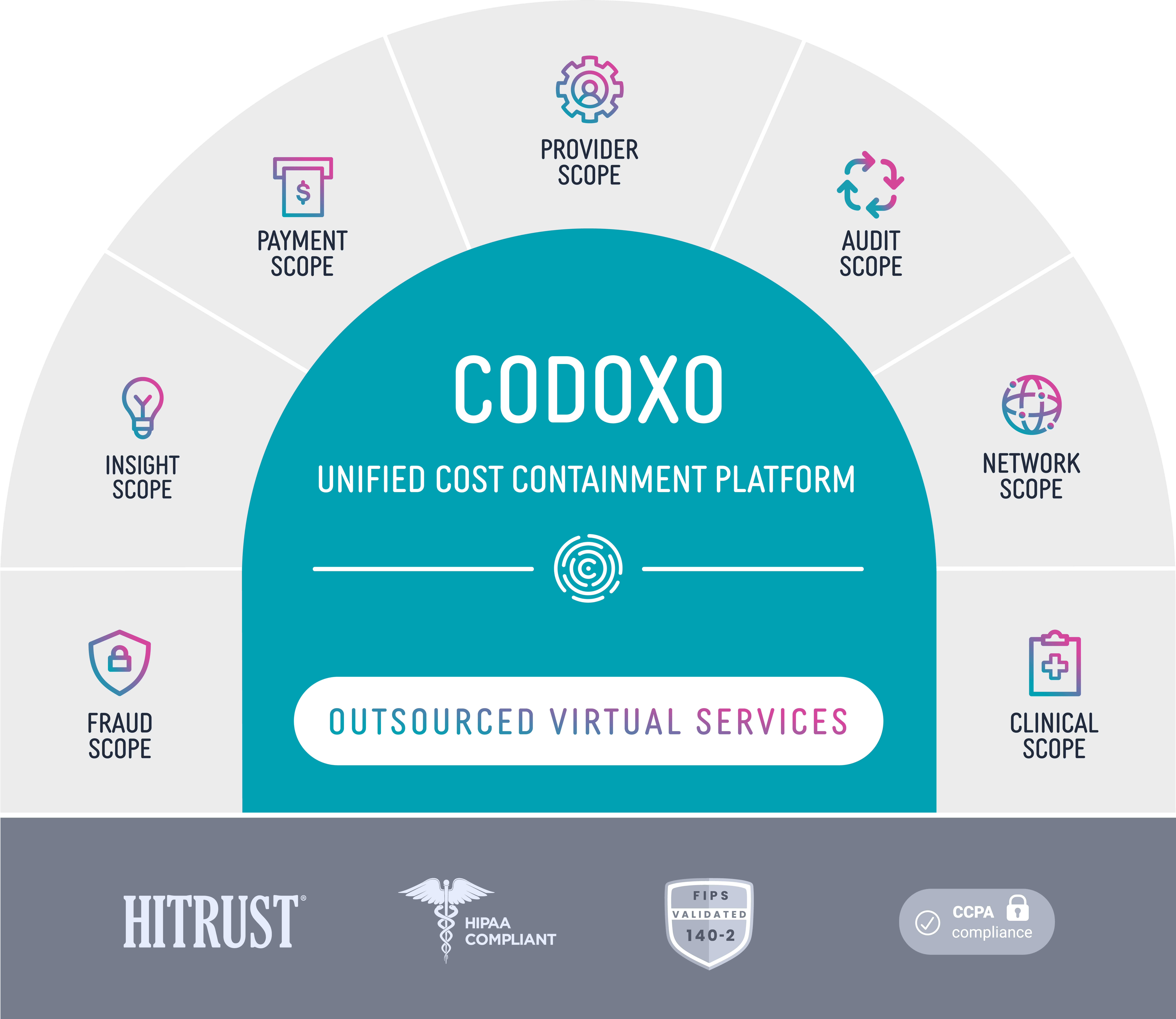
The Codoxo Unified Cost Containment Platform
Leading AI solutions for unified healthcare cost containment.
Smarter, faster, better.
Not all AI is created equal. Codoxo’s patented AI technology uses the most effective AI to ensure payment integrity as well as to anticipate and find fraud, waste and abuse issues our competitors cannot. Our remarkable speed to detection and deployment will help you stop the bleeding sooner for greater cost containment. Codoxo’s Unified Cost Containment Platform applies AI across the cost containment spectrum, including:
• Payment Integrity >
• Fraud, Waste, and Abuse >
• Provider Coding and Billing Education >
• Prior Authorization Acceleration >
• Network Integrity & Contract Management >
• Audit Case Management and Workflow >
• Outsourced Virtual Services >
Leading AI solutions for healthcare cost containment.
Smarter, faster, better.

Not all AI is created equal. Codoxo’s patented AI technology uses the most effective AI to ensure payment integrity as well as to anticipate and find fraud, waste and abuse issues our competitors cannot. Our remarkable speed to detection and deployment will help you stop the bleeding sooner for greater cost containment. Codoxo’s Healthcare Integrity suite applies AI across the cost containment spectrum, including:
The Codoxo Healthcare Integrity Suite
1 billion
CLAIMS
PROCESSED
$500M
SAVINGS
%
FALSE POSITIVES
%
INCREASE IN
PRODUCTIVITY

We invest heavily in our people and our technology to help us push the boundaries of what’s possible.
We have helped achieve savings at world-class payers and healthcare agencies including:
Highmark
6+ million members
State Medicaid Agency
1.5+ million recipients
Southeast Health Plan
3.5+ million members
Pacific Health Plan
700k+ members
Mid-State Health Plan
3.5+ million members
Midwest Plan
2.5+ million members

We invest heavily in our people and our technology to help us push the boundaries of what’s possible.
We have helped achieve savings at world-class payers and healthcare agencies including:
Highmark
6+ million members
State Medicaid Agency
1.5+ million recipients
Southeast Health Plan
3.5+ million members
Pacific Health Plan
700k+ members
Mid-State Health Plan
3.5+ million members
Midwest Plan
2.5+ million members

– Kurt Spear, Vice President Financial Investigations and Provider Review
HIGHMARK

– Kurt Spear, Vice President Financial Investigations and Provider Review
HIGHMARK
Resources
Ready for a better solution?
Request a demo to learn what we can do for you.
